Care ABC – I for Incontinence
Incontinence is as old as humanity itself. As early as the Ebers Papyrus – one of the oldest medical documents in the world, written around 1550 BC – ancient Egyptian physicians described the “dribbling of urine” and searched for treatments. What was recognized as a medical problem almost 3,600 years ago is still burdened with unnecessary shame today.
It doesn’t have to be that way.
Incontinence affects millions of people worldwide – statistically, half of all women experience some form of urinary incontinence during their lifetime. But it is not a failure of the body, rather a medical reality for which there are more solutions in 2026 than ever before. Professional care for incontinence today combines state-of-the-art aids with sensitive therapeutic methods to fully preserve quality of life.
This guide gives you everything you need right now: basic medical knowledge, practical everyday tips, product comparisons, and a clear overview of financial support in Austria and Germany.
Find support with discretion!
You care for a relative and are looking for an experienced professional who can support the topic of incontinence with expertise and dignity? noracares connects you directly with qualified caregivers.
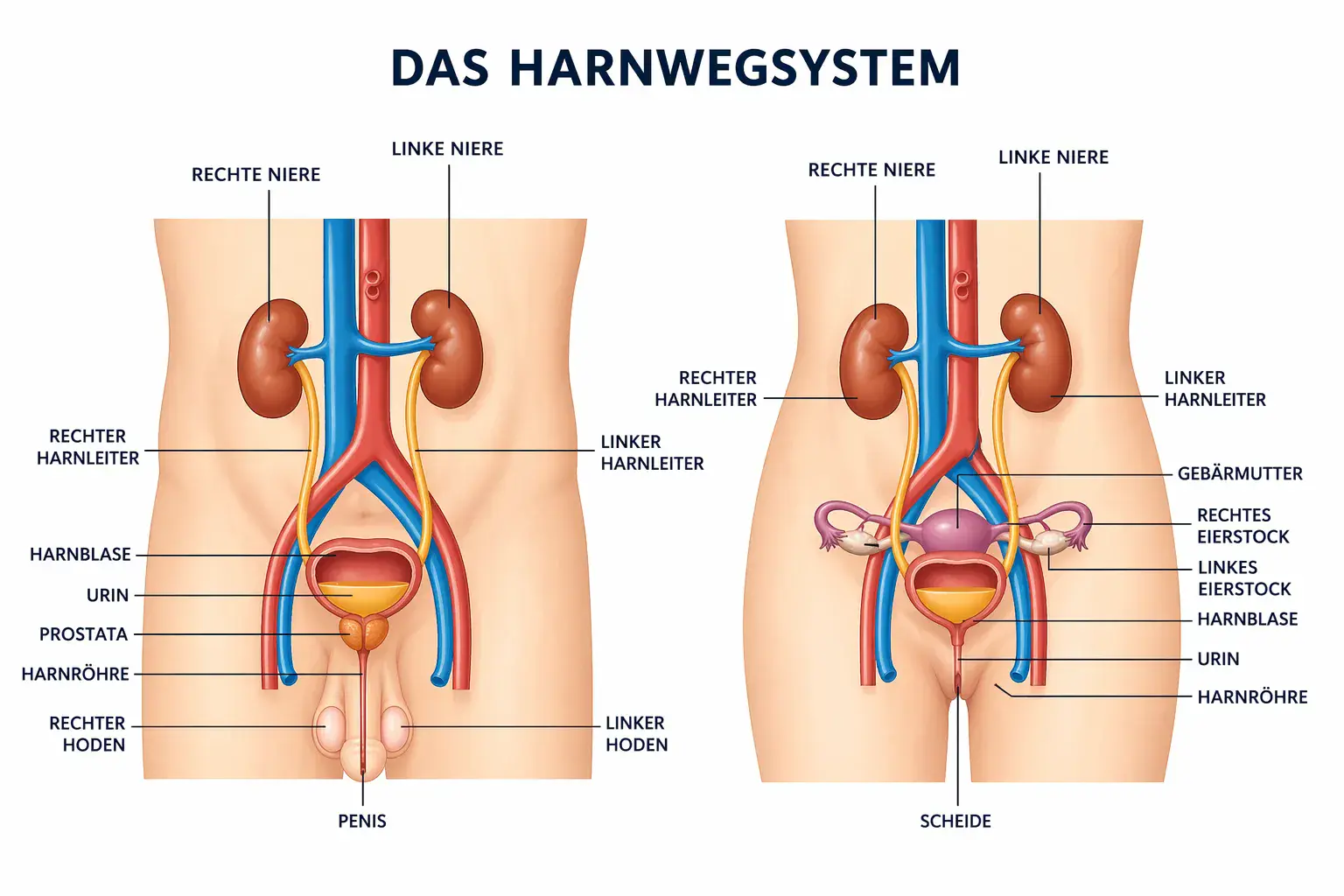
Incontinence refers to the inability to consciously retain urine or stool until the desired moment. It is not a disease in itself, but a symptom – a signal from the body that the interaction of muscles, nerves, and organs is disrupted. Causes can include physical changes, neurological impulses, or hormonal fluctuations.
Although statistically incontinence occurs more frequently in old age, it is not a “normal” part of aging. It affects people in all phases of life:
- Younger women: Often after pregnancy and childbirth (pelvic floor weakness).
- Men: Often after prostate surgery or with chronic inflammation.
- Patients with chronic conditions: As a result of diabetes, obesity, or neurological diseases such as Parkinson’s and multiple sclerosis.
The invisible vicious circle
According to the World Health Organization (WHO), urinary incontinence is one of the most underestimated health challenges worldwide. The problem is often not only physical hygiene, but also the psychological burden.
Many affected people withdraw out of shame: they avoid social contacts, give up hobbies, and risk loneliness or depression. In 2026 we know: the earlier the topic is addressed openly, the greater the chance of regaining full social participation through targeted training or modern aids.
It is important to understand that “incontinence” is an umbrella term. Depending on the cause, care and treatment differ dramatically.
Urinary incontinence
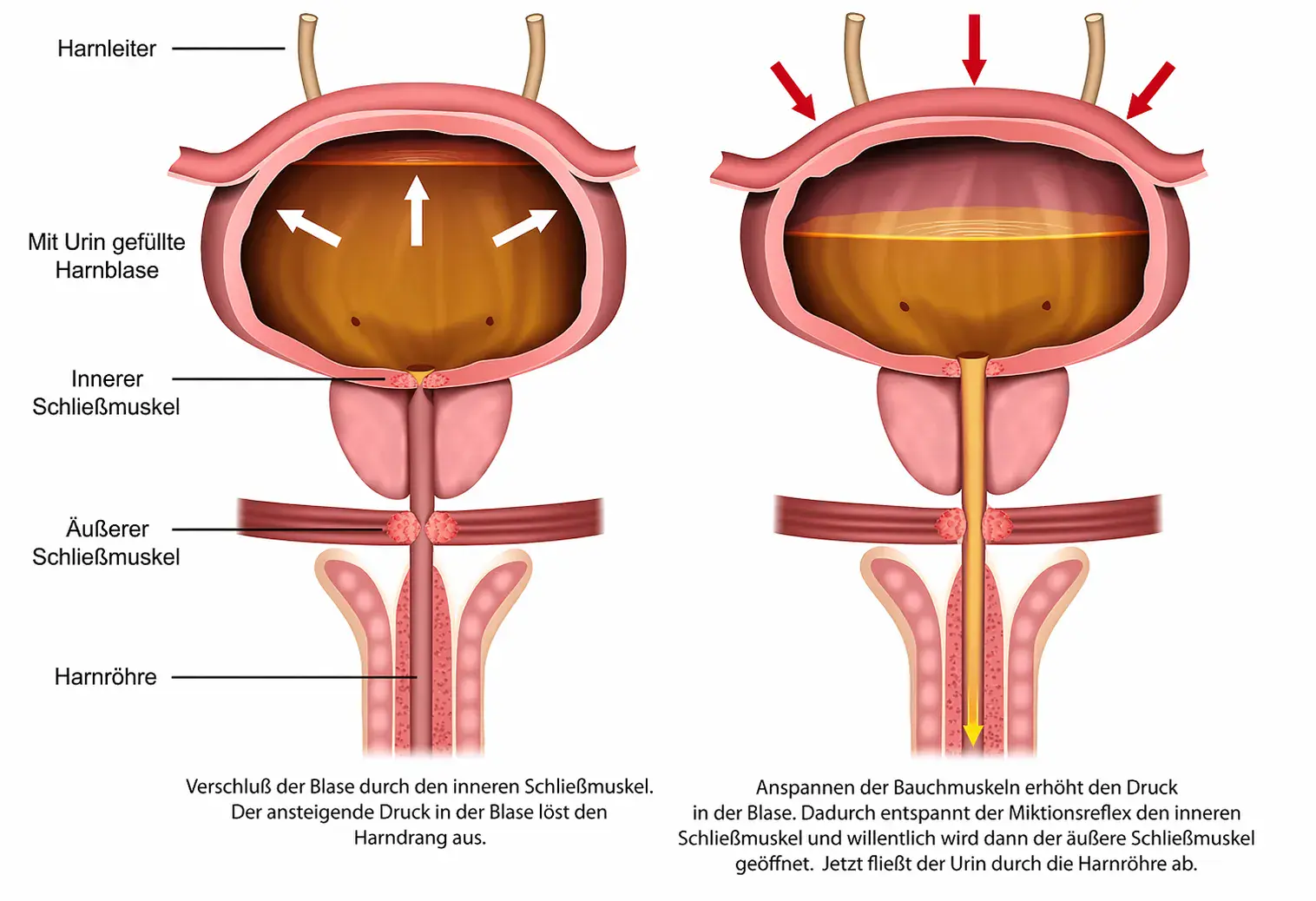
Urinary incontinence occurs when the bladder muscles, the sphincter, or the controlling nerves no longer work together harmoniously.
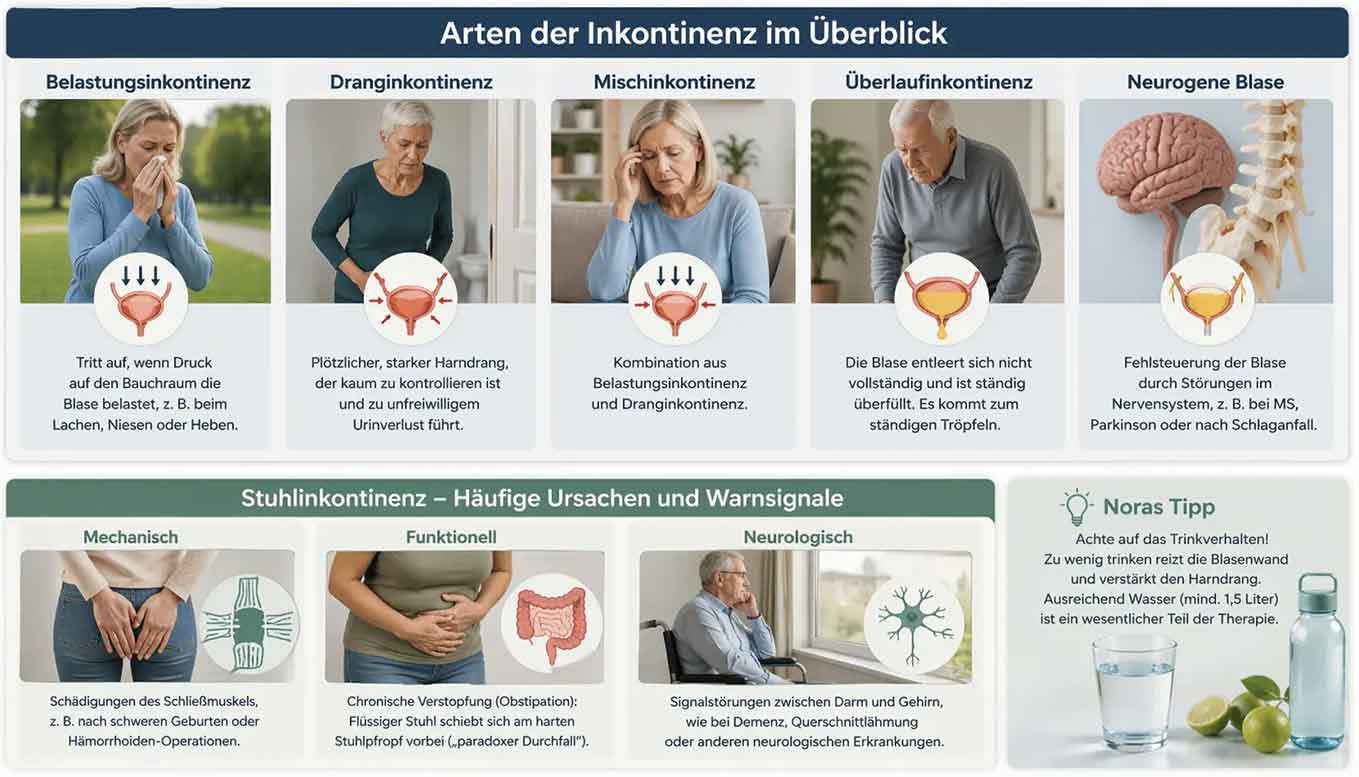
Types of urinary incontinence and their characteristics
Fecal incontinence
Fecal incontinence (bowel incontinence) is often even more associated with shame than urinary incontinence. In this case, the passage of gas or stool can no longer be controlled.
Common causes and warning signs:
- Mechanical: Damage to the sphincter (e.g. after difficult births or hemorrhoid surgery).
- Functional: Chronic constipation (obstipation). In this case, liquid stool moves past the hard stool blockage – this is often mistakenly interpreted as diarrhea ("Paradoxical diarrhea").
- Neurological: Signal disruptions between the bowel and the brain, as often occur in advanced dementia or paraplegia.
We are writing the year 2026, and incontinence care has changed radically. Away from purely passive "absorbent care" toward active, technological solutions that give affected people back their freedom.
1. The “bladder pacemaker” (SNM) – Now standard therapy
Sacral neuromodulation (SNM) is fully established in clinical practice in 2026. A small implant sends gentle electrical impulses to the sacral nerves and thus corrects the faulty communication between the brain and bladder.
- Fact 2026: In Austria and Germany, SNM is now a standard benefit of health insurance for patients with therapy-resistant urge incontinence. Success rates are over 80%.
- Your advantage: No more need for lifelong medication with side effects such as dry mouth or dizziness.
2. Intelligent sensors (IoT) – Dignity through data
Incontinence products in 2026 are "smart". Small, reusable sensors (often only the size of a coin) are attached to the outside of the pants or pads.
- Fact 2026: The sensors measure saturation level and temperature in real time. Via a secured app, the caregiver or family member receives a discreet notification on the smartphone before the product leaks or the skin is damaged.
- The "noracares" effect: The constant, often uncomfortable questions ("Is everything dry?") are eliminated. Changing happens exactly when it is necessary – this conserves resources and preserves privacy.
3. Biofeedback & digital therapy apps (DiGA)
Incontinence apps are fully reimbursable in 2026 as "Digital health applications" (DiGA) .
- Interactive training: Special pelvic floor trainers connect to the smartphone via Bluetooth. Patients can see their training progress live in the app (gamification).
- Prescription: Doctors in Germany and Austria can prescribe this "app on prescription," so that the costs for high-quality training devices and software are covered.
Structured management helps you regain control and preserve your relatives' skin health in the long term. The goal is to create security without limiting quality of life.
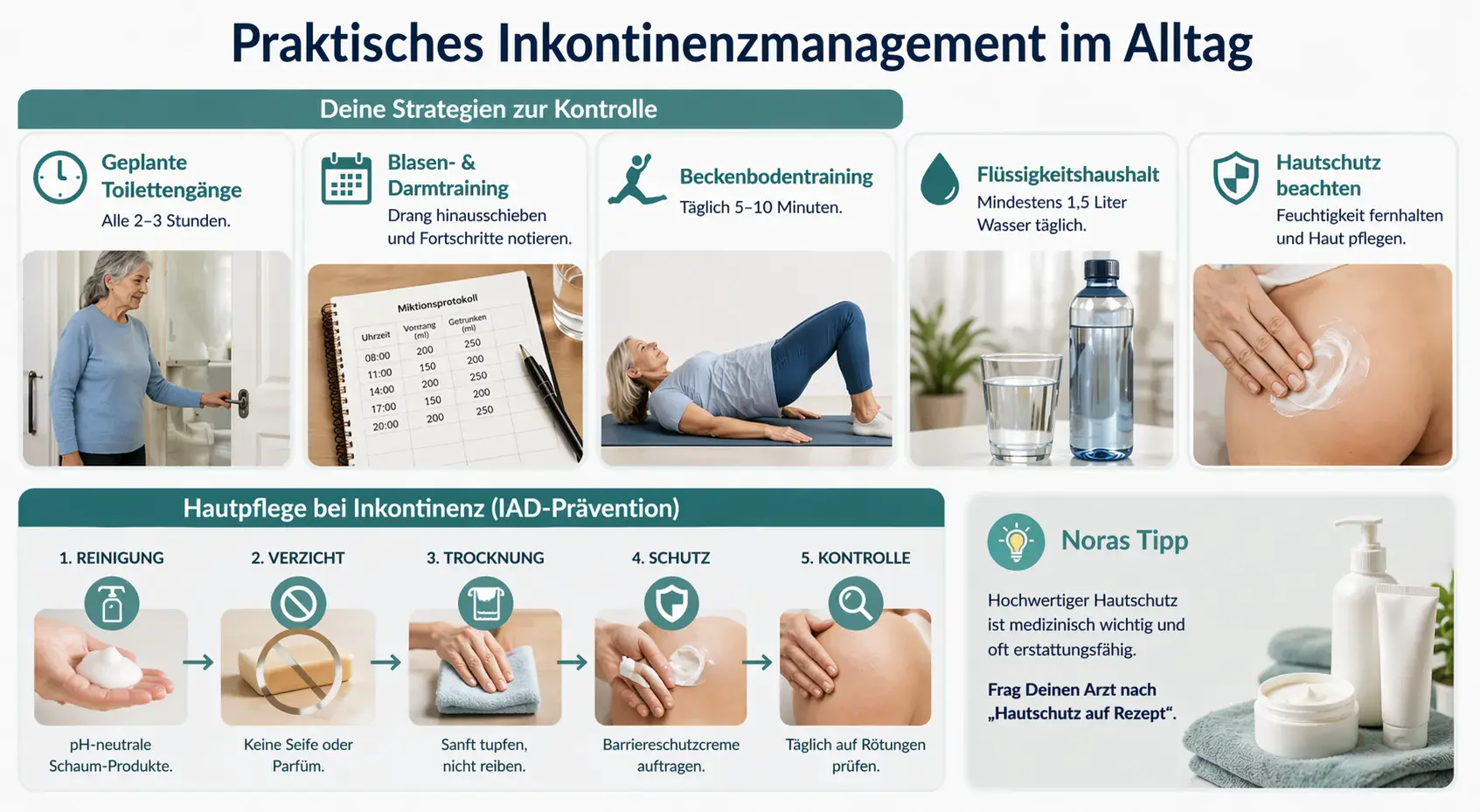
Your strategies for controlling incontinence
- Scheduled toilet visits: Regular visits every 2 to 3 hours – even without an urgent need – reduce the risk of accidents and train bladder capacity.
- Bladder and bowel training: By consciously delaying the urge to urinate by just a few minutes at first, nerve-muscle communication is strengthened. A voiding diary helps you document your progress objectively.
- Pelvic floor training: Kegel exercises are still the basic therapy in 2026. Daily training of just 5 to 10 minutes often shows significant success after only one month.
- Fluid balance: A daily intake of at least 1.5 liters is absolutely necessary. Many people make the mistake of drinking less to feel "safer" – but concentrated urine strongly irritates the bladder wall and only worsens incontinence even more.
Skin care for incontinence (IAD prevention)
The incontinence-associated dermatitis (IAD) is a painful inflammation caused by constant contact with urine and stool. With the right care system, you can avoid it almost completely.
Your standard for daily skin care
Choosing the right product determines comfort, skin health, and your relatives’ self-confidence. There is no universal solution – the product must match the degree of incontinence and lifestyle.
Overview of absorbent products
Day vs. night: adapting the rhythm
- During the day: Your focus here is on discretion and freedom of movement. In 2026, modern pants or pads are so thin that they are not noticeable under normal clothing. They enable an active life without fear of odors or stains.
- At night: Here, absorbent capacity is what matters. Special night products have a reinforced absorbent core in the rear area (for back sleepers) and protect the skin for many hours so your relatives (and you) can sleep peacefully.
Focus on material compatibility
When choosing, look for breathable, hypoallergenic materials without fragrances. In modern care in 2026, we avoid plastic-film products because they cause heat buildup and soften the skin.
Your next step toward relief
Are you caring for a relative with incontinence and noticing that you’re reaching your limits? You don’t have to manage this alone. noracares connects you directly with qualified caregivers who are professionals in incontinence management – discreet, experienced, and without expensive agency fees.
This is the most important question for many families: Who pays for all of this? The good news is that in 2026, a large portion of the costs for high-quality incontinence products and treatments is covered by health insurance companies and the care allowance.
Austria: how cost coverage works
In Austria, you are entitled to benefits in kind if there is a medical necessity.
- The medical prescription: Your first step is to go to your general practitioner. They will issue a prescription. Make sure that the exact diagnosis and the required absorbency level are noted.
- Use contract partners: With this prescription, you go to an orthopaedic technician or medical supply store that is a contract partner of your insurer (ÖGK, SVS or BVAEB). There, you often receive the products free of charge or for a small copayment.
- Care allowance as a basis: If incontinence is part of a broader need for care, the care allowance secures the financing.
Care allowance in Austria (as of 2026)
(Source: Adjusted values according to the Ministry of Social Affairs/PVA as of 2026)
Germany: assistive device allowance and care allowance
In Germany, care provision is regulated through the directory of medical aids. In addition to benefits in kind (products), from care level 2 onward you are also entitled to a monthly care allowance that you can use freely.
1. The incontinence allowance (benefit in kind)
The health insurance company pays a fixed monthly amount to a contracted supplier. This supplier delivers the basic care products directly to your home. If you want “premium products” (especially thin or breathable), you only have to pay the difference (additional payment).
2. Care aid subsidy
From care level 1 onward, you are additionally entitled to 40 euros per month for consumable care aids (such as disposable bed protection pads, gloves, or disinfectants).
3. Care allowance in Germany (as of 2026)
The care allowance is paid out when relatives or volunteers provide care at home. It can be used freely to finance support (e.g. via noracares).
(Note: The amounts correspond to the statutory adjustments for 2025/2026.)
Your path to reimbursement in Germany:
- Confirm the diagnosis: The doctor issues a “long-term prescription” (usually for 6–12 months).
- Choose a supplier: Contact your health insurance provider to find out which medical supply stores are contracted partners.
- Request samples: Insist that the supplier provide free samples so you can check the fit before the monthly flat rate is billed.
In 2026, quality in care is no longer shown only by “keeping someone dry,” but by actively promoting continence. The goal is to maintain independence for as long as possible.
The expert standard “Continence Promotion in Care”
In Germany and Austria, this standard is the binding benchmark for professional practice. Since the latest update (2024/2025), it explicitly includes both urinary and fecal incontinence.
What this standard requires of your caregiver in 2026:
- Systematic screening: Every care process begins with an assessment of the risks. If signs are overlooked, quality of life declines drastically.
- Continence profiles: Instead of simply saying “incontinent,” profiles are created. The goal is always to reach the next higher level of continence (e.g. from “incontinent with assistance” to “continent with support”).
- Person-centered planning: You and your relatives are part of the team. Measures are agreed on together, not decided over your heads.
- Skin integrity as a focus: The skin is protected as an organ. The goal is the combination of intact structure and full functionality.
Your standards for everyday care in 2026
Professional caregivers at noracares work according to these guidelines to safeguard dignity and health:
Professional quality checks in daily practice
Incontinence does not have to determine daily life. Often, it is small, strategic changes in the environment and routine that make the difference between isolation and an active life. These adjustments help your loved ones maintain their independence:
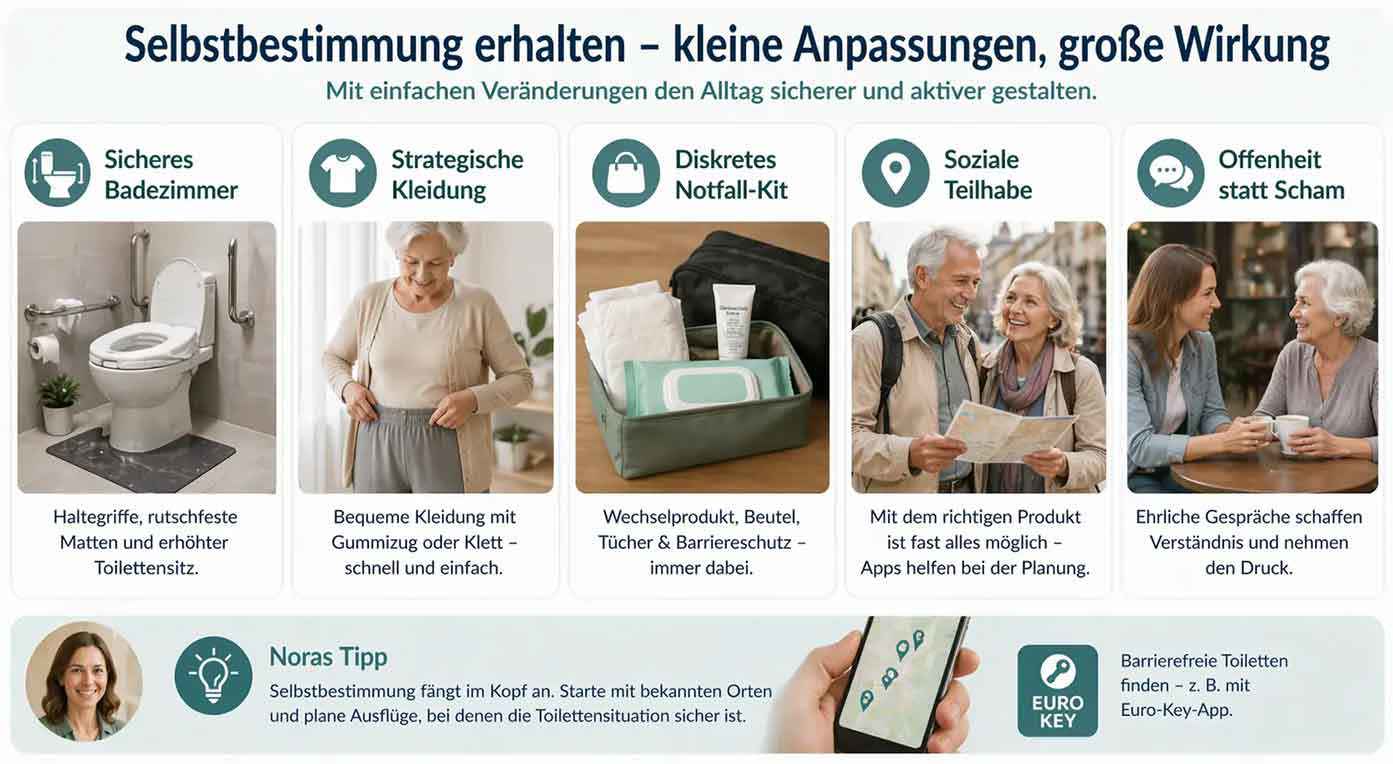
- Create an accessible environment: Design the bathroom so that it conveys safety. Grab bars in the right places, non-slip mats, and a raised toilet seat shorten reaction time and prevent falls during urgent trips.
- Choose clothing strategically: Clothing with elastic waistbands or Velcro fasteners instead of complicated buttons and zippers makes quick toilet visits much easier. There is now specialized care clothing that is functional and modern at the same time.
- The discreet emergency kit: Prepare a small, inconspicuous bag for when you are out and about. Contents: a fresh replacement product, odor-proof disposal bags, cleansing wipes, and a small tube of barrier cream. This provides reassurance on outings.
- Promote social participation: With the right product, almost anything is possible — from going to the theater to traveling. In 2026, there are apps that show accessible toilets near you (e.g. the Euro-Key system). Use these digital tools to plan your route.
- Openness instead of shame: Shame often consumes more energy than an honest conversation. If you and your loved ones speak openly about needs — whether in a restaurant or with friends — it reduces pressure and creates understanding.
Incontinence is not a modern phenomenon — it has accompanied humanity for thousands of years. But what has fundamentally changed is how we deal with it: in 2026, we have deeper knowledge, more discreet products, and more comprehensive support options than ever before.
One thing, however, must never change: The dignity of the person who needs help.
Whether you are caring as a relative, working as a professional, or are affected yourself — you have the right to the best possible support. The facts for 2026 are clear: financial assistance is anchored in law, high-quality products are reimbursed, and professional, compassionate care is accessible.
You do not have to walk this path alone. At noracares, you will find experts who support this topic with the necessary expertise, absolute discretion, and deep empathy.
Ready for professional support?
noracares connects you directly with experienced caregivers in Austria and Germany who guarantee incontinence care with dignity and professional competence — transparently, without agency fees, and without detours.
- Incontinence care – The entirety of nursing measures for the dignified, hygienic, and skin-friendly care of people with urinary or fecal incontinence.
- Bladder training – A technique for gradually extending the time between toilet visits in order to improve bladder control.
- Pelvic floor training (Kegel exercises) – Targeted muscle exercises to strengthen the pelvic floor and improve bladder and bowel control.
- IAD (Incontinence-associated dermatitis) – Inflammatory skin reaction caused by prolonged contact with urine or stool. Avoidable through consistent skin care.
- Expert standard for continence promotion – Binding nursing guideline in Germany and Austria for systematic continence assessment and individual support planning.
- Sacral neuromodulation (SNM) – A minimally invasive implant procedure that sends electrical impulses to sacral nerves and regulates bladder function – also called a “bladder pacemaker.”
- Incontinence flat rate – In Germany, the flat-rate reimbursement of incontinence aids by statutory health insurance funds following a medical prescription.
- Care allowance (AT) / care level (DE) – State financial support for people with a permanent need for care. Divided into 7 levels in Austria and 5 levels in Germany.
- Continence advisor – A specially trained professional in incontinence management – offers free or insurance-funded advice on products, training, and aids.
- Neurogenic bladder – Bladder dysfunction caused by nerve damage, e.g. in MS, spinal cord injuries, or diabetes.
Legal notice
All information is based on available sources and reflects the status of April 2026. This article is for informational purposes only and in no way replaces professional medical advice, diagnosis, or treatment. For binding information on individual cost coverage or the classification of care allowance, please contact your responsible health insurance provider or pension insurance institution directly.