Violence in Caregiving I: Your Shield as a Caregiver – Recognize, De-escalate & Act
Perhaps you remember a moment that hit you deeply. A degrading comment from a relative that went below the belt. A patient who hit or spat at you in a state of delusion. Or a workday when the pressure of the system was so massive that you barely recognized yourself anymore.
Violence in care happens. Often quietly, sometimes gradually – and yet it leaves deep scars. Current surveys from spring 2026 show: Almost every second caregiver in Germany and Austria experienced psychological or physical assaults in everyday professional life last year.
This is not an occupational risk that you simply have to “put up with.” This is a reality that must be taken seriously.
This article is your professional shield. It gives you the knowledge to clearly name violence, safely de-escalate situations, and know your rights exactly. Because one thing is clear: Your safety is the foundation of good care. Professionalism does not mean silently enduring everything – it means setting boundaries.
You are not alone with your experiences
In the noracares community, you will find a safe space for genuine exchange, mutual support, and guidance among colleagues who understand your situation.
Violence in care is not an isolated event, but a complex phenomenon. It refers to any action – whether actively carried out or by omission – that endangers the physical or emotional well-being of people in need of care or caregivers.
In 2026, experts agree: Violence is not a one-way street. It can come from caregivers, but also from people in need of care, relatives, or the institution itself (structural violence).
The official definition: The World Health Organization (WHO) defines violence in the care context as: “A single or repeated act or failure to respond appropriately within a relationship of trust, causing harm or distress to a person.”
Important for you as a caregiver:
In 2026, the legal framework in the EU has become stricter. Violence is no longer accepted as a “circumstantial aspect” of dementia or as an “occupational risk.” Naming a situation as violent is not a sign of weakness or lack of professionalism, but the legal prerequisite for your self-protection.
The three levels of violence in 2026
To understand the situation in Austria, Germany, and the EU holistically, we now divide violence into three dimensions:
- Interpersonal violence: Direct assaults between two people (e.g. a resident hits a caregiver or a caregiver restrains a resident without authorization).
- Institutional/Structural violence: Violence that arises from the system. Staff shortages, time pressure, and a poor error culture often force caregivers into situations where they have to act against their own ethical standards.
- Domestic violence in the care context: Due to the EU-wide harmonization of violence protection laws in 2026, violence by caregiving relatives (often due to overload) has come into stronger focus and gives you as a mobile caregiver more legal leverage during home visits.
Violence is far more than physical assaults or loud shouting. It often appears subtly – through ignoring, humiliation, boundary violations, or through the burden that a flawed system imposes on you. Understanding these forms is your most important tool for protecting yourself and others.
Forms of violence in everyday care as of 2026
Structural violence – The invisible perpetrator in the system
In 2026, this form is talked about more than ever. If today you have to care for 12 residents with severe care needs on your own, that is not a "stressful day" – it is structural violence.
This system pressure wears down your empathy. It leads to you perhaps grabbing more quickly or answering more harshly than you actually want to. It is important to understand: That does not make you a bad person, but it puts you in an impossible situation that provokes violence (including against yourself).
Take your safety back into your own hands.
No one should have to work under conditions that wear down their own empathy. At noracares, you decide how and where you work. Find families and work environments in which respect and time for people are not luxury goods, but the standard.
Violence in care almost never breaks out without a reason. It is often the sad end of a chain of pressure, exhaustion, and the feeling of being left alone.
When the system breaks you: The limit
Imagine it is Tuesday morning. You barely slept because you are worried about your own rent or your child is sick. You come to work and learn: Two colleagues have called in sick. Once again.
At that moment, your heart sinks. You know that today you cannot be the caregiver you want to be. You will run, you will have to say "no," you will have to compromise on the dignity of those in your care just to manage the workload. This is the breeding ground for violence.
What the pressure does to us
"That’s just part of it" – The most dangerous lie
Even in 2026, old beliefs persist stubbornly. When you hear: “Don’t be so sensitive, the patient is just confused,” violence is being normalized. But an insult remains an injury, even if it comes from a sick person. And a rough grip from you remains a boundary violation, even if you are under stress.
Nora’s heartbeat moment: Feeling overwhelmed is not failure. It is your soul’s emergency brake. In a world that keeps spinning faster, the highest form of professionalism is to say: “I just can’t do any more right now.” Only if you protect your own boundaries can you preserve the dignity of others.
Sabine’s story: The moment when the world stood still
Sabine loves her job. Or rather: she loved it. Today is one of those days when she asks herself why she is still doing this. There has not been a single free weekend for three weeks.
She is with Mrs. M., a resident with advanced dementia, whom Sabine actually cares about very much. But Mrs. M. is frightened today. She does not understand why she has to be washed, she screams and lashes out. Out in the corridor, the bell is ringing nonstop. Sabine is thinking about the medications she still has to prepare and the mountain of documentation on the table.
Her pulse is racing. She feels a heat rising inside her that frightens her. When Mrs. M. pushes her away again, Sabine loses control for a second. She grabs Mrs. M.’s thin arms a little too tightly, her voice hard and loud: “Now please keep still at last!” She yanks the shirt over her head. Mrs. M. falls silent immediately and looks at Sabine with large, watery blue eyes full of fear.
In that silence, Sabine collapses inside. This is not her. This is never who she wanted to be.
What saves Sabine:
In the past, Sabine would have swallowed this incident and cried alone at home in the evening. But today she breaks the silence. During handover, she says in a trembling voice: “Something happened to me today that I am sorry about. "I was at the end of my strength.”
Instead of being met with reproach, something magical happens: her colleagues nod. They know this abyss. Together they decide that Sabine will support another ward for the rest of the day to gain some distance. She uses the offer of supervision to learn how to recognize this “red zone” earlier. Sabine has learned: The first step against violence is naked honesty with yourself.
Violence has many faces, but it always leaves traces. Sometimes these traces are visible on the skin, but often they are hidden deep in the soul – in those you care for and in yourself.
Warning signs in those you care for
When a person you care for changes, it is often a silent cry for help. Pay attention to the subtle signals:
- Physical signs: Unexplained bruises (hematomas) in unusual places (such as the insides of the upper arms), small burns, or pressure marks that do not fit the medical condition.
- The language of fear: A sudden flinch when touched, avoiding eye contact, or a noticeable fear of certain people or situations.
- Withdrawal into silence: When a previously sociable person suddenly falls silent, refuses food, or stares blankly into space.
- Neglect: Hair is unkempt, clothes are dirty, or the skin is sore – signs that necessary care and attention are missing.
- Clear words: Never dismiss statements like “I am afraid” or “Please don’t hurt me” as mere confusion. They are the most honest form of feedback.
Warning signs in yourself
It is no shame to reach your limits. But it is dangerous to ignore the warning signals from your own body and mind. Be honest with yourself if you feel the following:
- Physical protest: Your body says “No” through chronic headaches, tension, sleep disturbances, or that leaden feeling of exhaustion as soon as you wake up.
- Emotional coldness: You notice yourself pulling away internally. You become cynical (“It doesn’t matter anyway”), indifferent, or feel an unusual impatience that could turn into aggression.
- Feeling of helplessness: The thought of giving up is your constant companion. You feel trapped in a hamster wheel and can no longer see a way out.
- The loud conscience: You are startled by your own reactions or words and carry heavy feelings of guilt with you, which drain even more of your strength.
Prevention does not mean making conflicts invisible, but making them manageable. If you have tools to steer tense situations, you protect not only the person in your care, but above all your own psychological and physical integrity.
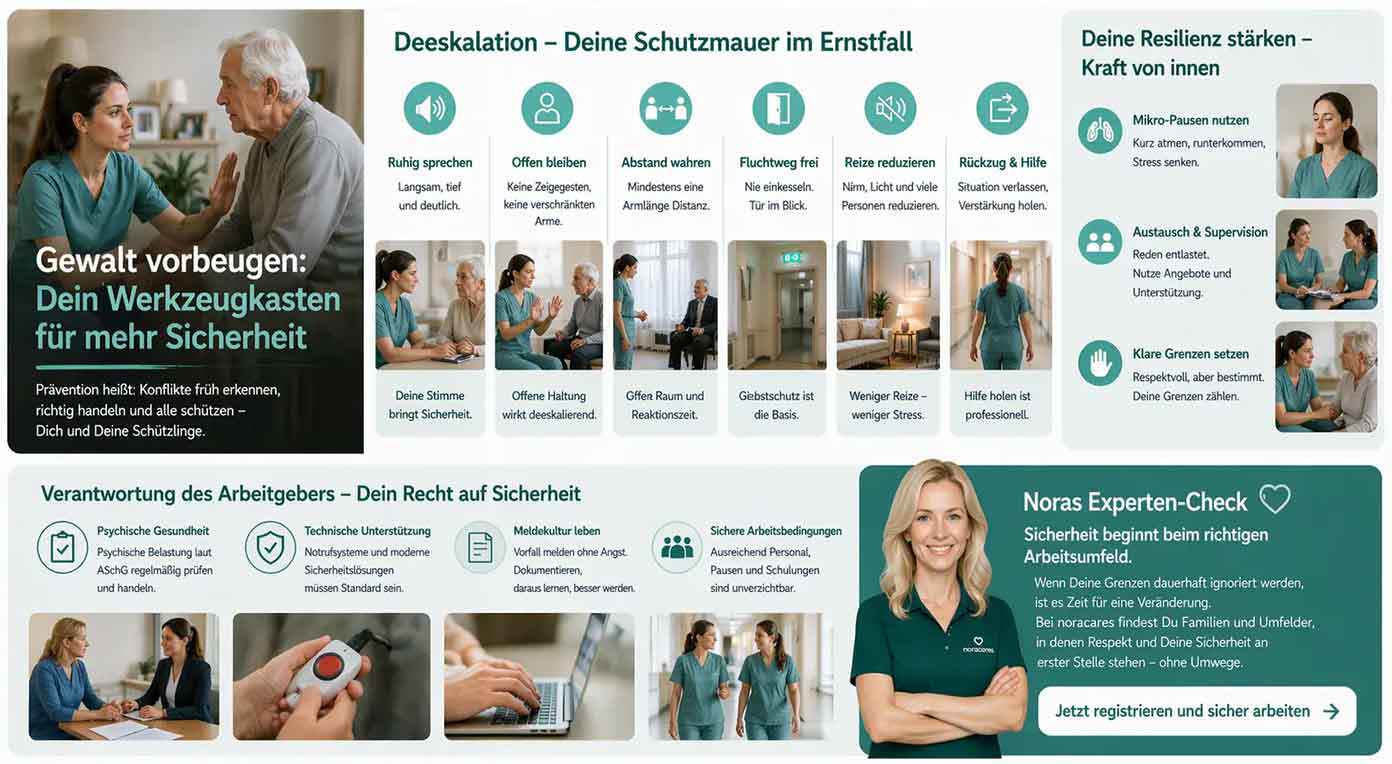
De-escalation – Your protective wall in an emergency
If a patient becomes aggressive – for example due to progressive dementia – de-escalation is your most important tool. It is not about “enduring” the situation, but actively calming it down.
Proven de-escalation techniques:
- Calm tone of voice: Speak slowly, deeply, and clearly. Your voice acts as a biological pacemaker: a calm frequency is unconsciously transferred to the other person and has a regulating effect.
- Body language as a signal: Avoid pointing gestures or crossed arms, as these may be perceived as threatening or defensive. An open, slightly sideways posture signals de-escalation and at the same time gives you better balance.
- Maintain a safe distance: Keep at least an arm’s length away. This gives the other person space and gives you the time you need to react to sudden movements.
- Prioritize an escape route: Make sure you never allow yourself to be “boxed in.” Always keep the way to the door open. Self-protection is the prerequisite for professional care.
- Reducing stimuli: Noise, bright light, or too many people present can fuel escalation. Minimal stimuli often lead to immediate relief for the nervous system.
- Controlled withdrawal: It is a sign of the highest professionalism to leave a situation when the danger becomes too great. Getting reinforcement is not failure, but responsible action.
Strengthening your resilience: Strength from within
- Micro-breaks for the nervous system: Just three minutes of focused breathing (e.g. the box breathing method) between visits to two rooms massively lowers your cortisol level and prevents you from carrying stress into the next encounter.
- Supervision and exchange: Use professional reflective discussions. In Austria, access to psychological counseling through the Chamber of Labour and nursing hotlines has been expanded further in 2026 to help prevent burnout caused by violence.
- Clear boundary-setting: You may and should set boundaries. A calm but firm “I do not want you to touch/speak to me like that” is a necessary part of shaping a professional relationship.
Employer responsibility – Your right to safety
Safety is not an individual achievement, but an organizational duty. A good employer in 2026 is characterized by proactively protecting your safety.
What a modern working environment must provide:
- Psychological evaluation: In Austria, the regular review of psychological stress is mandatory under the Employee Protection Act (ASchG). Make sure these results also lead to action in your workplace.
- Technical support: Functioning emergency call systems and modern safety concepts (e.g. de-escalation apps or smart buttons) must be standard.
- Error and reporting culture: A transparent reporting system without fear of sanctions is essential. Incidents of violence must be documented so the system can learn from them instead of looking for blame in the individual.
When a situation escalates, every second counts. A clear plan helps you remain capable of acting in an emotional emergency and protect yourself.
What to do when it happens?
Your right to refuse work
It is a widespread misconception that caregivers must endure everything. The opposite is true: In the event of acute danger to your health or safety, you have the right to refuse work in this specific situation – without having to fear labor-law consequences.
- In Austria: This right is anchored in the Employee Protection Act (ASchG).
- In Germany: The Occupational Health and Safety Act (ArbSchG) applies here.
Important for 2026: Document this step especially carefully. Note the date, time, the exact threat situation, and name witnesses. This documentation is your "airbag" if your actions are questioned afterward.
Points of contact: Here you can find help
If you experience or observe violence, do not hesitate to contact these specialized organizations. As of April 2026, these are the main points of contact:
Austria:
- Gewaltinfo.at: Central platform for information and counseling on violence in caregiving.
- Chamber of Labour (AK): Free legal advice and support for psychological stress in the workplace.
- WEISSER RING Austria: Professional help for victims of violent crime.
Germany:
- ZQP (Center for Quality in Care): Extensive resources and counseling guides on violence prevention (zqp.de).
- WEISSER RING e.V.: Nationwide support and victim helpline for people who have experienced violence.
- Telephone counseling: Anonymous and free counseling around the clock at 0800 111 0 111.
European Union:
- EU-OSHA: The European Agency for Safety and Health offers guides on dealing with violence and harassment in the workplace.
- EIGE: The European Institute for Gender Equality provides specific data and resources on gender-based violence in the healthcare sector.
Nora's final advice:
Keep this emergency plan in a place where you can find it quickly – perhaps even as a digital bookmark on your smartphone. In a real emergency, it is hard to think clearly; then this plan will guide you step by step back to safety. You deserve to be protected.
Your safety is the foundation!
Violence in care affects many people – and you have every right to call it by its name. It appears in physical assaults, in hurtful words, but also in overcrowded duty rosters and systems that demand the impossible from you. All of this leaves traces that you do not have to carry alone.
With knowledge, mindfulness, and the courage to set clear boundaries, you take the most important step for your own safety. Talk about what you are experiencing. Document incidents consistently. Get support – whether from colleagues, specialized counseling centers, or in the noracares community.
Never forget: looking after yourself is not a sign of weakness. It is the highest form of professionalism. Your safety is not negotiable – and neither is your dignity.
Stand up for your safety
Become part of noracares and shape your care workday in a self-determined, fair, and safe way. Here you will find direct contact with families and an environment that values your work – entirely without middlemen and system pressure.
- Violence in care – Any action or omission that causes harm or suffering to a person in the care context – physically, psychologically, sexually, financially, or through structural conditions.
- Structural violence – Harm caused by institutional processes: staff shortages, time pressure, lack of resources, or coercive measures. A form of violence exercised by the system.
- De-escalation – Targeted techniques to calm aggressive or dangerous situations – through voice, body language, distance, and environmental design.
- Resilience – Inner resilience that helps to cope with stressful situations without suffering lasting harm. Trainable through supervision, exchange, and self-care.
- Refusal to work – The legally enshrined right to refuse work in the event of acute danger to health or safety – without employment-law consequences.
- Documentation obligation – The obligation and at the same time the tool to document violent incidents completely in writing. Protects caregivers legally and enables traceability.
- Psychological violence – Harm through words, threats, humiliation, ignoring, or emotional neglect. Often underestimated, but with lasting consequences.
- ZQP – Center for Quality in Care (Germany). Central specialist organization for quality standards and violence prevention in care.
- ASchG – Employee Protection Act in Austria. Regulates, among other things, the right to safety in the workplace and the employer's duty to carry out psychological evaluation.
- Overwhelm – The feeling of no longer being able to cope with the demands of everyday care work. Often a precursor to burnout or unintentional boundary violations. Address it early.
Legal notice
All information in this article is based on the available sources and the state of knowledge as of April 2026.
This article is intended solely for general information and guidance. It does not constitute legal advice, medical diagnosis, or professional psychological counseling and cannot replace individual advice from experts (such as lawyers, psychologists, or victim protection organizations).
Important appeal: This text is purely an informational article. If you notice signs of violence – whether against yourself or against others – do not hesitate. Act immediately and seek professional help from the responsible authorities and specialist agencies in your country or region.
In case of acute danger, please contact the police or emergency medical services immediately:
- Austria: Police 133 / European emergency number 112
- Germany: Police 110 / European emergency number 112
- Throughout Europe: European emergency number 112