Care ABC – H for Heart Attack
A heart attack is not just a medical emergency – it also brings a wave of uncertainty and responsibility, especially for family members. When a loved one suddenly complains of chest pain or seems unusually exhausted, we often feel helpless. What can you do in this exceptional situation? And what happens next, when everyday life is suddenly shaped by medication schedules, doctor’s appointments, and concern for your loved one’s health?
This guide gives you clear answers – so you can act correctly in an emergency and provide meaningful support afterward. Because your informed, calm response can not only save lives, but also significantly influence recovery.
You do not have to walk this path alone!
Are you caring for a family member after a heart attack and need support? noracares connects you directly with experienced caregivers – simple, transparent, and with no hidden fees.
A heart attack (myocardial infarction) occurs when one of the coronary arteries suddenly becomes blocked – usually by a blood clot that forms on a plaque deposit. As a result, the heart muscle is no longer supplied with enough oxygen. If blood flow is interrupted for too long, heart muscle cells die irreversibly.
According to the World Health Organization (WHO) cardiovascular diseases remain the leading cause of death worldwide in 2026. In Europe, around 1.8 million people die from them each year, with heart attacks accounting for the largest share. In Austria and Germany, heart attacks are still among the most common causes of death, but the chances of surviving such an event well are higher today than ever before. Thanks to improved emergency response chains and modern diagnostics, the mortality rate has been steadily reduced in recent years.
A historical look: When was the heart attack discovered?
Heart problems have accompanied humanity for thousands of years – but the heart attack was only described as a clearly diagnosable medical condition in the 20th century. The Russian physician Nikolai Anitschkow laid the foundation for our current understanding of arterial calcification with his research on cholesterol and arteriosclerosis in the 1910s. James Herrick documented the first clinical description of an acute myocardial infarction in 1912.
Another milestone was the introduction of the electrocardiogram (ECG) by Willem Einthoven (Nobel Prize 1924). The ECG made cardiac arrhythmias and infarction patterns visible for the first time and revolutionized diagnosis.
Today, in 2026, this picture has changed again: while Einthoven’s device once filled entire rooms, your loved ones now wear ECG technology on their wrists as a smartwatch. Highly specialized cardiac catheter labs and AI systems that detect heart attacks in milliseconds ensure survival at a historically unprecedented level.
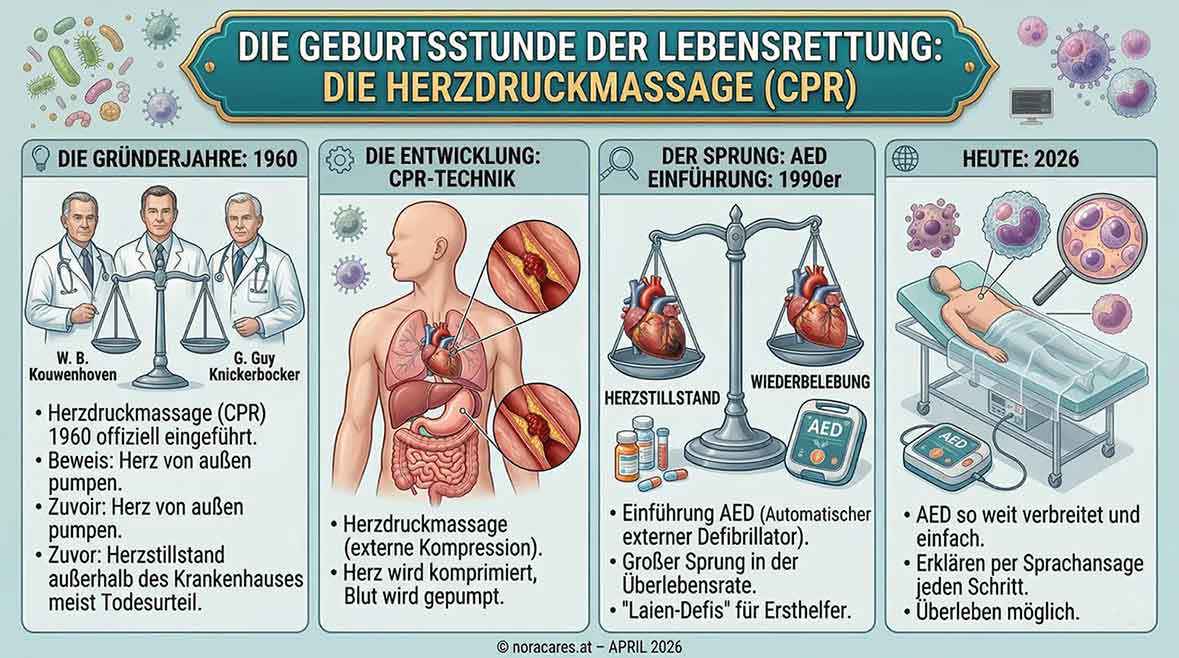
The birth of life-saving care: Chest compressions
Did you know that modern chest compressions (CPR) were only officially introduced in 1960? The researchers W. B. Kouwenhoven, James Jude, and G. Guy Knickerbocker proved at the time that a heart can be “pumped” from the outside. Before that, cardiac arrest outside a hospital was almost always considered a death sentence.
The introduction of the AED (automated external defibrillator) in the 1990s was the next major leap. Today, in 2026, these “public-use defibrillators” are so widespread and easy to use that they explain each step by voice instruction.
A heart attack does not always present with the classic severe chest pain. Especially in women, older people, or people with diabetes, the symptoms can be atypical or milder. Knowing this difference can save lives.
Typical symptoms in comparison
The faster action is taken, the greater the chance of survival – and the lower the damage to the heart. Never hesitate to call emergency services. Every minute counts.
This is how to act correctly – step by step
Step 1: Call emergency services immediately
- In Germany and throughout Europe (everywhere in the EU): 112
- In Austria: 144 (ambulance service).
- Tip : Use apps such as “Rettungshilfe” or your smartphone’s integrated emergency functions, which automatically send your location to the dispatch center via GPS.
Step 2: Calm the affected person
Speak calmly and clearly. Loosen tight clothing (tie, shirt button) to make breathing easier. Psychological support lowers stress levels and thus the heart’s oxygen demand.
Step 3: Raise the upper body slightly
Place the person in a semi-upright position (cardiac position). This mechanically relieves the heart and makes breathing easier.
Step 4: Do not leave them alone
Stay with the person until emergency services arrive. Continuously monitor their breathing and consciousness.
Step 5: If unconscious – start chest compressions
If the person does not respond and is not breathing normally (or is only gasping for air), you must act immediately. The procedure differs depending on age:
A. Adults (from puberty onward)
- Technique: Place both hands interlocked in the center of the chest.
- Compression depth: Press 5 to 6 cm deep.
- Rate: 100–120 times per minute (to the rhythm of “Stayin' Alive”).
- Ratio: 30 compressions, then 2 rescue breaths. If you are not trained in rescue breathing: “Hands-only” – simply keep pressing continuously.
B. Children (approx. 1 year to puberty)
- Technique: Depending on the child’s size, use one hand or both hands in the center of the chest.
- Special point: Since the cause in children is often a breathing problem, ideally begin with 5 initial rescue breaths before you start compressions.
- Compression depth: About one third of the chest diameter (approx. 5 cm).
- Ratio: 30 compressions, 2 rescue breaths.
C. Infants (under 1 year)
- Technique: Two-finger technique (index and middle finger) in the center of the chest, directly below the imaginary line between the nipples.
- Special point: Here too, begin with 5 gentle initial rescue breaths (mouth over BOTH the baby’s nose and mouth).
- Compression depth: About one third of the chest diameter (approx. 4 cm).
- Ratio: 30 compressions, 2 rescue breaths (gentle puffs).
Important note for 2026 (EU-wide): The guidelines of the European Resuscitation Council (ERC) emphasize for 2026: Do not stop! Keep pressing until the emergency services arrive (112 in the EU / 144 in AT) or the person shows clear signs of life again (defensive movements, opening eyes). If an AED (defibrillator) is available, switch it on immediately – it gives you exact spoken instructions for every age group (often with a child button/child electrodes).
Checklist: Emergency equipment for heart patients at home
So that you do not lose any time in an emergency, the following should be within easy reach:
- Emergency numbers & location: Clearly visible (e.g. on the refrigerator), including the exact address for emergency services.
- The digital emergency pass: Make sure the emergency pass (Health app) on your relative’s smartphone is filled out. Paramedics can read it directly in 2026.
- Current medication plan: Especially important for information about blood thinners.
- Find an AED (defibrillator): Do you know where the nearest “defib” is mounted? Many municipalities in AT and DE offer online maps or apps in 2026 that show the nearest AED location.
- First aid course: In Germany and Austria, many health insurance providers (such as ÖGK or Germany’s AOK) support special courses for family caregivers.
When it comes to the heart, the quality of the medical facility is a matter of life and death. In Europe, we are fortunate to have access to some of the world’s leading cardiology centers.
Austria: Excellence through networking
The Austrian Society of Cardiology (ÖKG) sets the high quality standards for the Alpine republic. Particularly important for you as a relative are the certified heart attack centers. These clinics guarantee 24/7 availability in the cardiac catheterization lab, which means specialists are on standby around the clock to reopen blocked vessels immediately.
Top clinics:
- Vienna General Hospital / MedUni Vienna: One of the largest and most renowned centers worldwide, with a focus on state-of-the-art cardiac surgery.
- Kepler University Hospital Linz: A leader in robot-assisted cardiac surgery.
- LKH University Hospital Graz: Specialized in complex cardiological interventions.
- Tyrol Clinics (Innsbruck): Excellent emergency care in the Alpine region.
Germany: The network of “Chest Pain Units”
In Germany, care is strictly regulated by the German Society of Cardiology (DGK). A milestone is the more than 300 certified Chest Pain Units (CPU). These specialized emergency departments are designed to clarify unclear chest pain within minutes.
Top clinics:
- German Heart Center of the Charité (DHZC): World-renowned for heart transplants and artificial heart support systems.
- Heart Center Leipzig: Specialist clinic with the highest case volume for minimally invasive valve procedures.
- Heidelberg University Hospital: A pioneer in translational cardiology (from research directly to the patient).
Important institution: German Heart Foundation – The most important place to go for patient information and clinic comparisons.
European Union: Common standards for your heart
The European Union ensures that heart medicine does not stop at national borders. Through the cooperation of leading institutions, it is ensured that a patient in Vienna receives the same excellent treatment as in Berlin or Paris.
- European Society of Cardiology (ESC): The scientific powerhouse based in Nice. The ESC guidelines are the “law” of modern cardiology. In 2026, the “ESC Clinical Excellence” seal is the gold standard for clinics that demonstrably integrate the latest research findings into daily clinical practice.
- European Alliance for Cardiovascular Health (EACH): This is the most important coalition of patient organizations, healthcare professionals, and industry at the EU level. Their goal for 2026: a common EU action plan for heart health to reduce mortality from heart attacks across Europe by 20%.
- European Health Data Space (EHDS): Instead of pilot projects, in 2026 the EHDS is the legal foundation. It makes it possible for vital patient data (such as ECG patterns and pre-existing conditions) to be shared anonymously across the EU. This feeds the AI early-detection systems, allowing them to learn to identify a heart attack in women or diabetics even more precisely.
- European Heart Network (EHN): This Brussels-based organization fights at the political level for the prevention of cardiovascular diseases throughout the EU.
Heart medicine is developing rapidly – and many of these innovations directly make daily caregiving at home easier.
1. AI-supported ECG analysis in real time
AI algorithms for ECG evaluation are in use in many European emergency departments in 2026 and recognize infarction patterns – including so-called “silent” heart attacks – significantly faster than conventional methods.
The European Society of Cardiology (ESC) has recommended the use of AI-supported diagnostic systems in acute cardiology in its current guidelines.
(Source: escardio.org and How AI is redefining the ECG | ESC Digital & AI Summit )
2. Wearables & patches: Heart monitoring in everyday life
Smartwatches and medical patch sensors can continuously monitor heart rhythm, atrial fibrillation, and other abnormalities. For relatives, this offers an important advantage: if values become critical, the device can automatically send a notification.
The ESC recommends monitoring via wearables for patients after a heart attack – especially for the early detection of atrial fibrillation.
Whether a specific device is approved as a medical product varies depending on the manufacturer and EU country. Ask your family doctor or cardiologist for advice on which device is suitable for your relative.
(Source: Wearables: Are smartwatches useful for heart patients? | Heart Foundation)
3. New medications: PCSK9 inhibitors and Inclisiran
PCSK9 inhibitors such as Evolocumab or Alirocumab are an important alternative for lowering cholesterol in high-risk patients who cannot tolerate statins. They are approved in Germany and Austria and are reimbursed by health insurance companies when appropriately indicated.
Inclisiran – an siRNA therapy that is injected only twice a year – has been approved in the EU for several years and sustainably reduces LDL cholesterol. For everyday caregiving, this means: no daily tablet intake, less forgetting, better adherence to therapy.
(Source: herzstiftung.de)
4. Telemedicine and digital patient records
In Germany, the electronic patient record (ePA) has enabled the structured digital transmission of vital signs to the treating practice since 2025. In Austria, ELGA (Electronic Health Record) is the corresponding infrastructure.
Blood pressure monitors and scales with digital connectivity can transmit measurements directly to the practice – in the event of critical deviations, the practice team contacts the patient proactively. (Please check for 2026: current availability and connectivity depending on the practice and region)
Important note on this section: The technologies mentioned are real and highly advanced in development – however, some details such as exact approval classes, reimbursement conditions, or product names can change quickly. We therefore recommend always coordinating specific product decisions with the treating cardiologist or family doctor.
Prevention is the most effective protection – today we call it “Active Heart Management.” The WHO and the ESC emphasize that up to 80% of heart attacks could be prevented by controlling risk factors.
The most important risk factors at a glance
Why 150 minutes of exercise?
For 2026, the WHO continues to recommend the “magic number” of 150 minutes of moderate physical activity per week. That is about 20 to 25 minutes per day – a brisk walk is often enough. Exercise not only lowers blood pressure, but also keeps the blood vessels elastic and “cleans” the arteries from the inside.
How to find specialists near you:
Choosing the right doctor is the first step toward safety. Use these proven portals:
- In Austria: The platform DocFinder.at is the first place to go to find cardiologists near you – including patient reviews and information on public or private practices.
- In Germany: Here, the KBV physician search (National Association of Statutory Health Insurance Physicians) or the portal Jameda.de offers a reliable search for specialized physicians and certified “Chest Pain Units.”
- In the EU: Via the website of the European Society of Cardiology (ESC) lcertified centers of excellence can be found throughout Europe. In addition, the EU patient portal provides information on cross-border healthcare.
How noracares supports you with prevention:
Prevention in old age is teamwork. Our caregivers at noracares support your loved ones in integrating these 150 minutes of exercise into everyday life, cook heart-healthy Mediterranean meals together, and ensure medication is taken on time. This turns prevention from a burden into a shared routine that provides security.
After discharge from the hospital, a crucial phase begins for you as a relative. Care requires patience, structure, and an alert eye for warning signs.
The phases of recovery
Daily routine: How to structure care at home
Morning routine – A good start to the day
- Measure and document blood pressure and pulse
- Give morning medication on time and with enough water
- Light breakfast – heart-healthy, low in salt
- Short exercise session (walking in the apartment or a short walk depending on the stage of recovery)
- Briefly ask about mood and well-being
Afternoon care – Step by step
- Keep a rest period – an afternoon nap if desired
- Check afternoon medication
- A small activity together – conversation, reading, looking at the garden
- Pay attention to fluid intake – at least 1.5 to 2 liters daily
- Watch for signs of exhaustion, shortness of breath, or restlessness
Evening routine – A calm ending
- Give evening medication
- Create a relaxed atmosphere – no stress, no exciting news
- Allow night rest – upright sleeping position in case of shortness of breath
- Brief documentation of the day (vital signs, condition, abnormalities)
Medication management after a heart attack
Consistent medication intake is one of the most important measures after a heart attack. Frequently prescribed medications are:
- Antiplatelet agents (e.g. aspirin, clopidogrel) – prevent new clots
- Beta blockers – protect the heart, reduce oxygen demand
- ACE inhibitors or ARBs – lower blood pressure, protect the heart
- Statins – lower cholesterol levels
- Aldosterone antagonists – for heart failure after a heart attack
Strengthening the heart: Nutrition after a heart attack
A heart-healthy diet is not a restriction – it is a gift to the heart.
The Mediterranean diet is considered especially heart-protective according to the ESC and WHO. It is based on lots of vegetables, legumes, fish, olive oil, and little red meat. For this heart-healthy change to succeed in everyday life, a helping hand is often needed.
You do not have to heal your family’s heart alone. Worrying about a loved one weighs heavily – let us carry part of that burden. At noracares, you will find not only expertise, but compassionate support that gives you the time to simply be a family member again.
Regular checks provide reassurance. Pay attention to every change – it can indicate complications.
Vital signs log: What you should measure daily
Warning signs – When to act immediately?
After a heart attack, many affected people experience anxiety, low mood, or depression. According to studies, up to 30 percent of heart attack patients develop depressive symptoms in the first weeks. (Source: ESC – Please check for 2026)
For the affected person
- Give space for fears and feelings – actively listen without judging
- Talk about the fear of a relapse – this fear is normal and justified
- Recommend psychological support or heart support groups
- In Germany: Cardiac exercise groups are funded by health insurance providers
- In Austria: Cardiac rehabilitation programs at specialized centers
For you as a caregiver
Care means responsibility – but not self-sacrifice. Take care of yourself too.
- Plan breaks – use outpatient services or 24-hour care
- Talk about it – exchange ideas with other family caregivers
- Get informed – care courses are offered by health insurance providers in Germany and Austria
- Get advice – care support centers (DE) and social counseling centers (AT) help you free of charge
If permanent limitations such as exhaustion or restricted mobility remain after a heart attack, you are entitled to support.
In Germany: The care level
You submit the application to the care insurance fund. Afterwards, the Medical Service (MD) assesses the degree of limitation.
In Austria: The care level
You submit the application for care allowance to the responsible pension insurance provider. An assessor determines the actual care needs.
Benefits at a glance
Care after a heart attack begins with understanding – and thrives on attentiveness, structure, and a lot of heart. As a relative, you make the crucial difference when you know what matters.
Today you have learned the tools: from quick response in an emergency to modern 2026 medication management and heart-healthy nutrition. This knowledge makes you more confident and gives your loved one quality of life. But don’t forget: Good care only succeeds when you also feel safe and supported.
Let’s make sure together that your family’s heart beats in balance again. At noracares you will find the professional and human support that makes exactly this difference.
Together, we can do this.
Ready for the next step?
You don’t have to walk this path alone. noracares connects you directly with qualified caregivers who specialize in cardiac care at home – transparent, personal, and without agency fees. Give your family the security it needs now.
- Atherosclerosis – Hardening and narrowing of the arteries due to plaque deposits. A central risk factor for heart attack and stroke.
- Cardiopulmonary resuscitation (CPR) – Life-saving measure in cardiac arrest. 30 compressions on the chest, then 2 breaths alternately. Standardized emergency procedure since 1960.
- Heart attack (myocardial infarction) – Death of heart muscle tissue due to sudden blockage of a coronary artery, usually caused by a blood clot.
- Nursing care / heart attack care –All caregiving measures after a heart attack: medication administration, monitoring of vital signs, nutrition, mobilization, and emotional support.
- Myocardium –The heart muscle, which is partially damaged by a heart attack.
- PCSK9 inhibitors –Modern class of medication to lower cholesterol, significantly reducing the risk of heart attack in high-risk patients.
- Plaque –Deposits of fat, cholesterol, and other substances on artery walls that can lead to narrowing and blockage.
- Statins –Group of medications used to lower LDL cholesterol. Standardly prescribed after a heart attack.
Thrombosis – Formation of a blood clot in a blood vessel that can obstruct blood flow and trigger a heart attack or stroke.
Vital signs – Measurable body functions: blood pressure, pulse, respiratory rate, body temperature, and body weight. Regular monitoring is essential after a heart attack.
All information is based on available sources as of March 2026. This article was created for informational purposes and does not replace medical advice. If symptoms persist, always consult your family doctor or emergency medical service.
Sources: who.int, escardio.org, okg.at, dgk.org, herzstiftung.de, gesundheit.gv.at, bundesgesundheitsministerium.de