Care ABC – C is for Cholesterol
Updated expert article | As of: February 2026
Cholesterol is a term that often causes concern – especially in old age. Suddenly, levels that used to be unproblematic begin to rise, and many questions arise: Which values are still normal? When is medication necessary? And how seriously does high cholesterol in old age really endanger health?
Cholesterol in old age is a topic that unsettles many people and their relatives. Peter, 74, loved his morning walks – until he suddenly suffered a heart attack caused by years of elevated cholesterol levels. It becomes clear: values that once seemed harmless can have serious consequences in later life. Women after menopause are particularly affected. At the same time, contradictory information circulates: Should cholesterol-lowering medication still be taken after 70? Which values are truly critical?
If you are asking yourself these questions, you are not alone. Many seniors – and their families – are looking for clear, understandable answers. In this article, you will find not only medical basics and current studies, but above all practical tips, age-appropriate reference values, and concrete recommendations on how to deal with elevated cholesterol in everyday life. This way, you can keep an eye on your health – without fear, but with knowledge and confidence.
For many, cholesterol is associated with the idea of fatty deposits in the arteries. But in old age, this term takes on a new meaning. The reasons are diverse and range from natural changes in the body to external influences. Let’s take a look at the most important factors that affect cholesterol levels in later life.
Overview: Cholesterol and metabolism in old age
Metabolic changes in old age: The body slows down
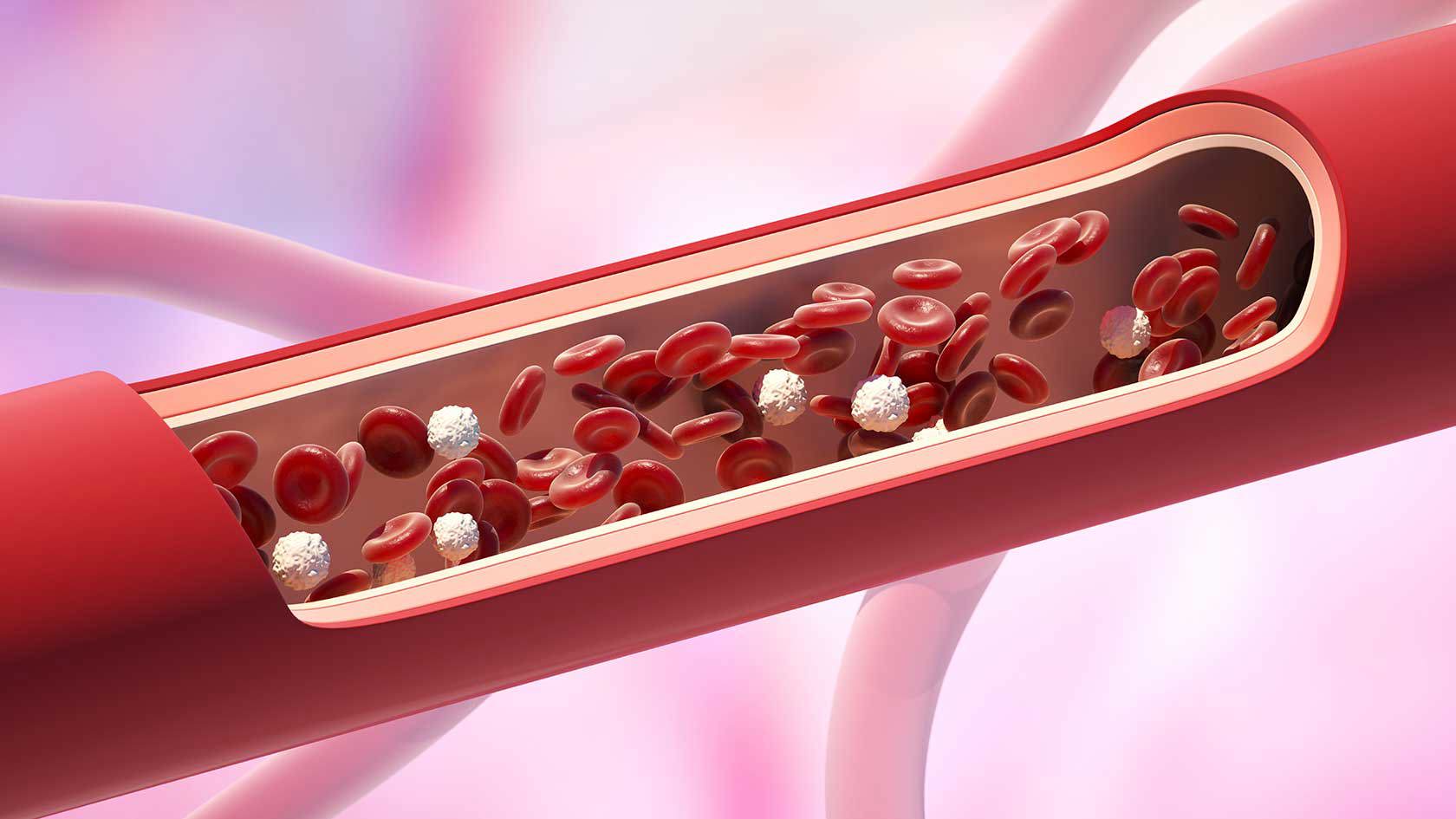
As we age, metabolism slows down. The body requires less energy, and the ability to efficiently process dietary fats decreases. As a result, excess cholesterol is no longer broken down as quickly and can accumulate in the blood. LDL cholesterol in particular, often referred to as “bad” cholesterol, rises and can deposit in the arterial walls, increasing the risk of cardiovascular diseases.
Hormonal changes: Menopause and its effects
In women, menopause plays a crucial role. The decline in estrogen levels leads to an increase in LDL cholesterol and a decrease in protective HDL cholesterol. These hormonal changes increase the risk of cardiovascular diseases. Studies show that menopause is associated with an increase in triglycerides and LDL cholesterol.
Comorbidities and risk factors: An interplay of factors
In old age, comorbidities such as high blood pressure and diabetes often occur, which can negatively influence cholesterol levels. Persistently high blood pressure can damage vessel walls and promote the deposition of cholesterol. In addition, insulin resistance, as occurs in diabetes, can disrupt fat metabolism in the body and lead to elevated cholesterol levels.
Genetic predisposition also plays a role. People with familial hypercholesterolemia have a reduced ability to remove cholesterol from the blood due to a genetic defect, which leads to elevated cholesterol levels.
Cholesterol is a vital building block of our body, but metabolism changes in old age. This makes it all the more important to know the recommended reference values.
Overview: Cholesterol levels by age group
The following tables show the reference values for people without known cardiovascular diseases*:
Women
These values serve as general guidance. Individual target values may vary depending on health status and risk factors. (ZAVA).
Cholesterol levels in women aged 60 and 70+
With menopause, many things change in the body, including fat metabolism. Due to decreasing estrogen levels, “bad” LDL cholesterol rises, while protective HDL decreases. The heart thus loses an important protective factor. Women over 60 therefore develop vascular calcification more frequently, often gradually and with different symptoms than men: instead of the typical chest pain, heart problems are more likely to manifest as fatigue, shortness of breath, or nausea. For this very reason, regular preventive check-ups and blood tests are especially important from this age onward.
Men
These values serve as general guidance. Individual target values may vary depending on health status and risk factors. (ZAVA).
Cholesterol levels in men over 60
In men, more visceral fat accumulates in the abdominal area with increasing age – a silent risk factor for the heart and blood vessels. LDL rises, arteries stiffen earlier, and many already carry past burdens such as high blood pressure or years of smoking. Close monitoring of cholesterol levels, combined with exercise and a balanced diet, helps prevent heart attacks and strokes – before the first symptoms even appear.
Why the table is only half the truth: Risk matters!
While the tables above provide a good initial classification, cardiologists today work according to the principle: The sicker the vessels, the lower the value must be. If you already have health issues to deal with, the standard value of 115 mg/dl is often not enough. Experts then recommend significantly lower LDL target values:
- With high risk (e.g., diabetes or severe high blood pressure): below 70 mg/dl.
- After a heart attack or stroke: below 55 mg/dl.
Cholesterol levels over 70 – What is still normal?
At 70+, levels often rise slightly as metabolism naturally slows down. Nevertheless, the rule is: If cardiovascular diseases are present, LDL today should be below 100 mg/dl or even below 70 mg/dl to prevent further plaque buildup. If you are otherwise completely healthy and have no vascular damage, your doctor will often view values around 115 mg/dl more calmly.
LDL, HDL and total cholesterol at a glance
Cholesterol is not simply “good” or “bad” – our blood carries different types that play different roles. Some help keep the vessels clean, others tend to deposit in the arteries. Knowing your levels helps you better assess what is currently happening in your body.
- Total cholesterol: This value represents the sum of LDL, HDL and other fat components (triglycerides). A value below 200 mg/dl is considered a good guideline for healthy seniors.
- LDL cholesterol: Often referred to as “bad” cholesterol because it can deposit in the arteries. While under 115 mg/dl is targeted for fit individuals, much stricter goals apply for high-risk patients (as described above).
- HDL cholesterol: The “good” cholesterol acts like waste disposal and transports fat away from the vessels. A value above 45 mg/dl (women) or 40 mg/dl (men) is the goal.
- Triglycerides: These “neutral fats” serve as an energy reserve. If they are consistently above 150 mg/dl, they can accelerate vascular calcification together with cholesterol.
Differences between men and women
The normal value depends on age and increases slightly with advancing years. In young women, it is generally somewhat lower than in young men. With increasing age, this difference evens out. Older women have, on average, higher cholesterol levels than older men. According to a study, the average total cholesterol level of people between 35 and 65 years in Germany was around 236 mg/dl (6.1 mmol/l) in the early 1990s.
In old age, it is therefore particularly important to check cholesterol levels regularly and adjust them if necessary. A healthy lifestyle with a balanced diet, regular exercise and, if necessary, medication can help keep levels in the optimal range and minimize the risk of cardiovascular diseases.
With increasing age, not only our lifestyle habits change, but also our body. Blood vessels become less elastic, deposits accumulate more easily, and cholesterol levels can rise unexpectedly. For many seniors, this remains unnoticed for a long time – until the first warning signs appear.
High cholesterol levels increase the risk of cardiovascular diseases, strokes and other health problems. Let’s look at some typical scenarios that show why cholesterol should be taken particularly seriously in old age.
Heart attack and stroke in old age
Peter, 74, loved his morning walks in the park. One day he suddenly felt a sharp pain in his chest and shortness of breath. His doctor diagnosed a heart attack – the result of years of elevated cholesterol levels that had built up as deposits in his coronary arteries.
Strokes are also a major risk in old age: In Maria’s case, 70, a significantly elevated LDL level combined with high blood pressure led to a minor stroke that temporarily limited her mobility. These examples show: Even seemingly “small” changes in the blood can have fatal consequences.
Arteriosclerosis and circulatory disorders
Clara, 68, noticed pain in her calves after walking just a few meters. The diagnosis: peripheral arterial disease (PAD), caused by narrowed arteries as a result of high cholesterol levels.
Such deposits impair blood circulation and not only cause pain, but also increase the risk of falls and injuries. Arteriosclerosis often progresses silently – you only notice the danger when blood flow is already severely restricted.
Connection with diabetes and other diseases
Johann, 75, has been living with type 2 diabetes for years. His high cholesterol level intensified the vascular strain that diabetes already causes. The combination of too much “bad” LDL cholesterol and high blood sugar led to accelerated vascular calcification, significantly increasing his risk of heart attacks and strokes.
Many seniors like Johann often realize too late how closely cholesterol, diabetes and other accompanying conditions are linked.
In old age, it is particularly important to keep an eye on cholesterol levels. Excessively high cholesterol can increase the risk of cardiovascular diseases. But don’t worry: With targeted measures, cholesterol levels can be positively influenced. Here you can find out how to take action.
Adjusting your diet: Swap instead of just giving up
Diet is one of the strongest levers for influencing cholesterol levels. Modern nutrition concepts focus less on radical restriction and more on deliberately replacing “bad” fats with heart-healthy alternatives.
The fat swap: Here’s how to do it easily
It’s less about the amount of fat and more about the type of fatty acids. Try to replace saturated fats (usually animal-based) with unsaturated fats (usually plant-based):
Your cholesterol helpers: Fiber & Omega-3
Some foods act like a natural “brush” for your blood vessels:
- Fiber (waste disposal): Especially soluble fiber from oats (beta-glucan), legumes, apples and berries binds cholesterol in the intestine and promotes its excretion.
- Omega-3 fatty acids: Fatty fish (salmon, mackerel) or flaxseed oil help lower triglycerides and improve blood flow properties.
- Plant sterols: These natural substances (e.g., in nuts or fortified foods) block the absorption of cholesterol from food.
Exercise and everyday tips
Regular exercise is another key factor. Even in old age, you can achieve a lot with gentle activities: walking, swimming or gymnastics are good for the body and heart. Try to be active for at least 30 minutes a day – even small steps add up and make a big difference.
Medication and therapy
Sometimes exercise and diet are not enough, and medication is necessary to lower cholesterol levels. Your doctor will decide together with you which therapy makes sense for you.
Statins in old age – Benefits and risks
Statins lower LDL cholesterol and reduce the risk of cardiovascular diseases. However, they can have side effects, such as muscle pain or digestive problems. Your doctor will clarify with you whether the benefits outweigh the possible risks.
Alternative therapies
If statins are not well tolerated or are not sufficient, there are other medications:
- Ezetimibe: Inhibits the absorption of cholesterol in the intestine
- PCSK9 inhibitors: Strongly lower LDL cholesterol
These medications are often used in addition to statins.
When is lowering cholesterol no longer worthwhile?
From around the age of 82, the benefit in prevention (primary prevention) is considered limited. If your life expectancy is reduced or your general condition is significantly impaired, discontinuing statins may make sense. However: Never stop medication on your own. This is always a joint decision with your doctor.
Important to know: Different rules apply to people who have already suffered a heart attack or stroke than to those who are completely symptom-free – in these cases, continuing therapy can still save lives.
For many senior women and men, it is not easy to give up long-standing eating habits. This is exactly where relatives and caregivers provide support in everyday life:
- Peter, 74, loved his morning walks, but breakfast remained a challenge. Thanks to the support of his everyday companion, who helps him with cooking together and meal planning, a bowl of oatmeal now regularly replaces bacon on the table. Preparing meals together turns the change into a social event rather than strict deprivation.
- Maria, 70, lost motivation to cook healthy meals alone after her minor stroke. Today, she prepares Mediterranean dishes with lots of vegetables and olive oil together with her caregiver. Chopping and cooking together not only improves her LDL levels but is also important training for her fine motor skills.
Implementing nutrition in everyday care
For many senior women and men, it is not always easy to eat healthily. This is where relatives and caregivers are needed: They can prepare meals that are high in fiber and cholesterol-lowering, for example whole grain bread, vegetable dishes or fish such as salmon and mackerel.
Peter, 74, loved his morning walks in the park, but his high cholesterol was already bothering him at breakfast. Instead of his usual sausage sandwich and bacon, thanks to his daughter he now regularly reached for a bowl of oatmeal with fresh fruit. These small, targeted changes to his diet quickly made a noticeable difference and helped slow the buildup in his coronary arteries.
Taking and monitoring medication correctly
Medication for high cholesterol, such as statins or alternative therapies, only works if it is taken regularly. Family members and caregivers can give reminders, monitor intake, and watch for side effects.
Maria, 70, had difficulty taking her medication correctly after a minor stroke. Her caregiver introduced a clear medication chart and checked her intake daily. This helped Maria keep her levels stable and reduce the risk of further strokes.
Exercise and motivation despite limitations
Exercise is crucial, even when physical limitations exist. Walks, light gymnastics, or water exercises help keep vessels flexible and positively influence cholesterol levels.
Clara, 68, noticed pain in her calves after just a few meters of walking due to her peripheral arterial disease (PAD). With the support of her caregiver, she was able to complete short walking distances every day and do stretching exercises. The motivation from having someone accompany her helped her stay active despite the pain – a key to improving circulation.
Keeping an eye on doctor visits and lab values together
Regular doctor visits and blood tests are essential for seniors to keep an eye on cholesterol levels, blood pressure, and blood sugar. Family members can coordinate appointments, document lab values, and report any abnormalities immediately.
Johann, 75, has been living with type 2 diabetes for years. His caregiver regularly goes with him to check-ups, notes the lab values, and then discusses them with the doctor. This helped Johann better understand the interaction between diabetes and cholesterol and take targeted countermeasures.
Putting it into practice day to day – healthy meals, on-time medication, regular exercise – is often the biggest challenge. If you need support to keep your loved one’s cholesterol levels under control, clarify your care situation free of charge in 3 minutes.
noracares is not just an expert in theory: We support you directly with practical implementation in everyday care and help ensure that nutrition, exercise, and medication are reliably carried out.
Making everyday implementation easier – use professional placement services
Putting it into practice day to day – healthy meals, on-time medication, regular exercise – is often the biggest challenge. noracares helps you find the right support: We connect you with qualified professionals who accompany you directly with practical implementation in everyday care – whether with heart-healthy cooking or as motivating companions for daily exercise.
Cholesterol in old age is more than just a lab value – it is an important signal that should be taken seriously, without causing fear. As we age, metabolism, hormones, and lifestyle habits change. That’s why it’s crucial to check the values regularly, discuss them individually with your doctor, and choose suitable measures together.
What’s important is this: There isn’t one single right path for everyone. For some, medication is the main focus; for others, an adjusted diet, exercise, or simply consciously weighing quality of life against health benefits. Family members and caregivers can be a valuable support in this – whether with cooking, doctor’s appointments, or reminders to take medication.
The good news: Even at an older age, there’s still a lot you can do for your heart and blood vessels. With clear information, practical tips, and support that fits your personal situation, you can ensure that cholesterol doesn’t remain a bogeyman, but rather a well-controllable part of your health.
- Atherosclerosis (hardening of the arteries): A chronic condition in which fats (cholesterol) and calcium build up in the artery walls. This leads to narrowing, which can cause circulatory disorders, heart attack, and stroke.
- Ezetimibe: A medication that inhibits the absorption of cholesterol from the intestine. It is often used when statins alone are not sufficient or are not tolerated.
- HDL cholesterol (High-Density Lipoprotein): Often referred to as “good” cholesterol. It acts like a “garbage collection service” for the vessels, transporting excess cholesterol back to the liver where it is broken down. High HDL levels protect the blood vessels.
- Cardiovascular risk: The probability of suffering a disease of the cardiovascular system (e.g., a heart attack) within a certain period of time. This risk largely determines today how strictly cholesterol levels need to be controlled.
- Comorbidities: Technical term for accompanying conditions, i.e., the simultaneous occurrence of two or more chronic illnesses (e.g., diabetes and high blood pressure) that influence each other.
- LDL cholesterol (Low-Density Lipoprotein): Often referred to as “bad” cholesterol. It transports cholesterol to cells, but in excess it can deposit in the arteries and promote hardening of the arteries.
- Lipid profile: A detailed laboratory blood test that breaks down all relevant lipid values (total cholesterol, LDL, HDL, and triglycerides) to better assess individual risk.
- PAD (Peripheral arterial occlusive disease): A circulatory disorder that usually affects the legs. It is often triggered by atherosclerosis and leads to pain, especially when walking (“shop window disease”).
- Primary prevention: Prevention of diseases before they occur at all (e.g., lowering cholesterol in otherwise healthy people).
- Secondary prevention: Measures to prevent things from getting worse or a relapse after an existing illness (e.g., after a first heart attack). Particularly strict LDL target values apply here.
- Statins: One of the most commonly prescribed groups of medications for lowering LDL cholesterol. They inhibit the body’s own cholesterol production in the liver.
- Triglycerides: Neutral fats in the blood that serve as an energy store. If they are persistently elevated, they represent another important risk factor for cardiovascular disease alongside cholesterol.